The following information is courtesy of Deborah Freudenmann has a Bachelor of Health Sciences in Naturopathy and is a co-author and teacher of the Functional Medicine Health Coaching program
Let’s dive into the world of colon cancer—a significant health concern that affects countless lives. Colon cancer ranks as the third most common cancer-related cause of death in the United States. Colon cancer takes root in the large intestine affects 1 in 23 men and 1 in 25 women at some point in their life. In this article, we’ll learn about colon cancer, explore its signs and symptoms, delve into its root causes, understand treatment options, and arm you with natural strategies to support your well-being.
Why Is A Functional Medicine Approach to Cancer Important
The Functional Medicine approach to cancer takes a comprehensive and holistic view of the disease. Unlike traditional medical models that often focus solely on treating symptoms, Functional Medicine seeks to identify and address the root causes of cancer.
In this paradigm, cancer is not viewed as an isolated event but as a complex interplay of genetics, lifestyle, environment, and individual health factors.
This approach prioritizes prevention through lifestyle modifications such as nutrition, stress management, and physical activity. It also emphasizes optimizing the body’s natural detoxification processes, supporting the immune system, and reducing chronic inflammation—factors known to influence cancer risk and progression.
Functional Medicine practitioners may use advanced diagnostic tools to uncover imbalances or deficiencies in the body, allowing for targeted interventions.
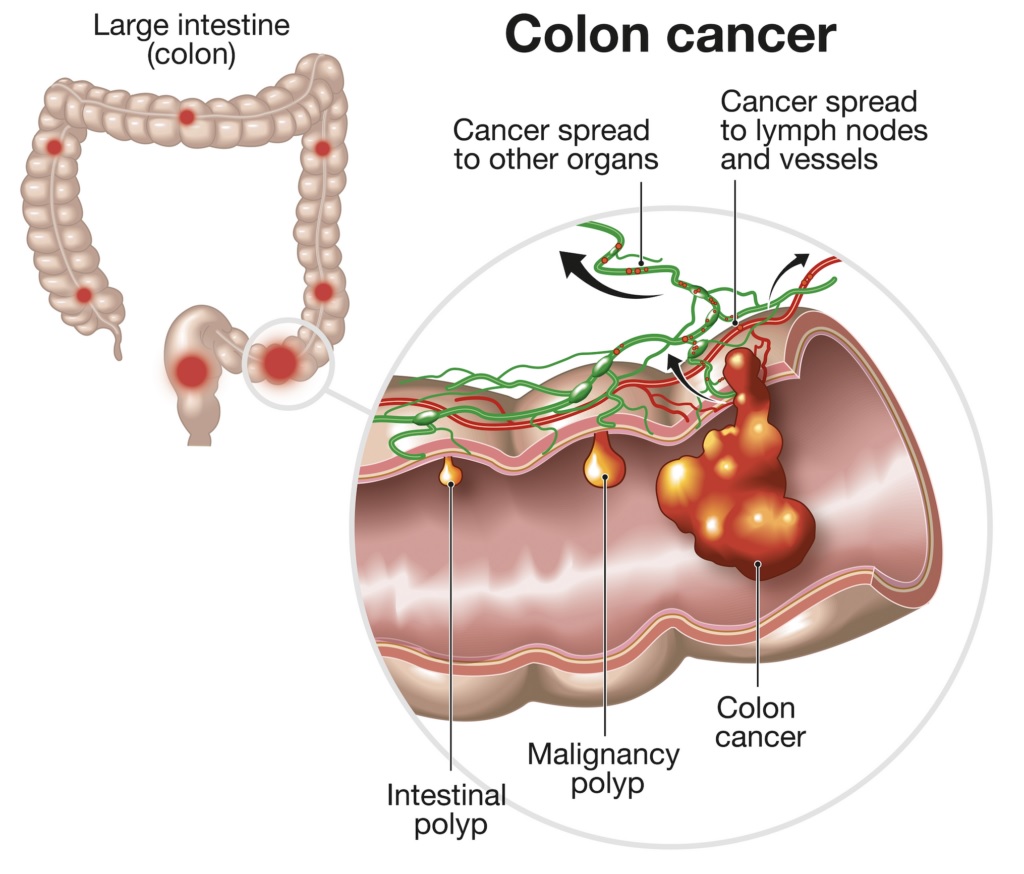
What is Colon Cancer
Colon cancer, often grouped under the broader term colorectal cancer, originates in your colon or large intestine—a vital organ responsible for extracting water and salt from solid waste. These remnants then venture into the rectum, the last six inches of your large intestine, before being expelled through your anus. While colon cancer sets its sights on the colon, its cousin, rectal cancer, focuses on the rectum. Nevertheless, these two often intertwine or spread across each other’s domains.
The numbers speak volumes: the American Cancer Society reports over 104,000 new cases of colon cancer and 45,000 new cases of rectal cancer annually. A stark reality is that 1 in 23 men and 1 in 25 women will grapple with colorectal cancer in their lifetime. Disturbingly, it stands as the third most common cause of cancer-related fatalities in the United States. The risk tends to surge with age, prompting healthcare experts to recommend routine screening post the age of 50.
Signs and Symptoms
Colon cancer comes with a slew of potential indicators:
- Changes in bowel habits: This could manifest as constipation, diarrhea, or narrow stools, persisting for more than a few days.
- Rectal bleeding: If you notice bright red blood in your stool, it’s a cause for concern.
- Dark stools: Blood in the stool may cause it to appear dark brown or black.
- Unresolved bowel movement urgency: The persistent feeling of needing to relieve yourself even after doing so.
- Abdominal discomfort: Unexplained abdominal pain or cramping.
- Anemia: Unexplained anemia, weakness, fatigue, or unintentional weight loss.
While these symptoms can trigger anxiety, it’s essential to remember that they can also be linked to other issues, including hemorrhoids, infections, irritable bowel syndrome (IBS), or inflammatory bowel disease (IBD), stress affecting your digestive system.
Colon Cancer Risk Factors
Colon cancer is influenced by a whole host of factors, some of which are beyond our control, while others offer room for intervention. Age, family history, and ethnicity belong to the former category, while lifestyle choices, diet, toxins, and alcohol consumption fall into the latter. For those predisposed to higher-risk categories beyond their control, vigilance regarding modifiable factors such as diet and lifestyle are important.
Consider these factors contributing to colon cancer risk:
- Age: The risk escalates significantly after the age of 50.
- Personal and family history: A history of adenomatous polyps or colon cancer increases vulnerability.
- Inflammatory bowel disease: Conditions like Crohn’s disease or ulcerative colitis elevate the risk.
- Genetic inheritance: Certain genetic syndromes, including Lynch syndrome and familial adenomatous polyposis (FAP), heighten susceptibility.
- Racial and ethnic background: Being Black or of Ashkenazi Jewish descent increases risk.
- Health conditions: Type 2 diabetes, obesity, and sedentary living can be contributing factors.
- Dietary choices: Overconsumption of processed meats, low fibre intake, processed foods etc.
- Vitamin D levels: Low levels of this vitamin are a potential risk factor.
- Smoking: Cigarette smoking is linked to an elevated risk.
- Alcohol consumption: Heavy alcohol use may contribute to the risk.
Conventional Approaches to Colon Cancer
A range of conventional treatments are available for colon cancer, these include surgery, radiofrequency ablation, cryosurgery, chemotherapy, radiation therapy, targeted therapy, and immunotherapy. The choice of treatment depends on the stage and grade of the cancer.
Surgery: It entails removing cancerous tissue from the colon.
Radiofrequency ablation: This method employs tiny electrodes to eliminate cancer cells.
Chemotherapy: This treatment employs drugs to halt cancer growth and eradicate existing cancer cells.
Radiation therapy: High-energy x-ray radiation targets and destroys cancer cells. It can be delivered internally or externally.
Understanding Some Of The Root Causes
Colon cancer’s origins are multifaceted, involving health conditions, lifestyle choices, and nutrition. Here are some of the primary root causes:
Chronic Inflammation
While inflammation is a normal response to injuries and infections, chronic inflammation, fueled by factors like diet, obesity, environmental toxins, stress, and poor sleep, can lead to cancer. The National Institute of Health (NIH) notes that chronic inflammation can result in oxidative and DNA damage, paving the way for cancer. Individuals with chronic inflammatory bowel diseases are also at heightened risk.
Obesity and Insulin Resistance
A significant portion of the U.S. population suffers with obesity and insulin resistance. Both conditions are associated with an increased risk of colon cancer. Insulin resistance impedes the body’s ability to respond effectively to insulin and manage blood glucose levels, escalating the risk of prediabetes and diabetes.
Chronic Stress and Poor Sleep
These twin culprits contribute to chronic inflammation, fostering an environment conducive to colon cancer development. Stress at the molecular level is intertwined with inflammation, although further research is needed for a comprehensive understanding. Moreover, inadequate sleep duration has been linked to an elevated risk of colon cancer.
Smoking and Heavy Alcohol Use
The American Cancer Society underscores that both smoking and heavy alcohol consumption can heighten the risk of colon cancer. Smoking exposes the body to harmful chemicals and toxins, contributing to DNA damage and cellular mutation. Excessive alcohol use also raises the risk.
High Toxic Load
Exposure to environmental toxins can significantly increase the risk of colon cancer. Occupational exposure to substances like asbestos and arsenic has been associated with elevated risks. Additionally, pesticides and mycotoxins present in the food supply are pertinent concerns.
Chronic Infections and Gut Dysbiosis
The health of your gut plays a pivotal role in overall well-being, and in the context of colon cancer, it’s of paramount importance. Chronic gut infections and imbalances in gut microbiota can substantially elevate the risk. Parasitic infections and dysbiosis have both been linked to colon cancer development.
Vitamin D Deficiency
Inadequate levels of vitamin D are recognized as a significant diet and nutrition-related risk factor for colon cancer. This vital nutrient has been shown to play a role in the prevention and treatment of colon cancer.
Natural Strategies for Support
Empowering yourself with proactive, natural strategies can be instrumental in reducing your risk of colon cancer and supporting overall health.
Anti-Inflammatory Nutrition
Chronic inflammation is a known risk factor for colon cancer. Adopting an anti-inflammatory diet by eliminating inflammatory foods like refined sugar, refined oils, gluten, artificial additives, and processed meats while prioritizing nutrient-rich options such as vegetables, low-glycemic index fruits, and healthy fats can promote a balanced internal environment.
Stress Reduction and Improved Sleep
Mitigating chronic stress and enhancing sleep quality are vital steps in reducing inflammation and supporting overall health. Practices like meditation, yoga, journaling, and relaxation techniques can aid in stress management. Establishing a calming bedtime routine can significantly improve sleep quality.
Physical Activity
Regular physical activity is pivotal in maintaining a healthy weight and reducing the risk of colon cancer. Incorporate exercises that encompass cardiovascular workouts, strength training, and low-impact activities into your routine. Even simple activities like walking and stretching can make a difference.
Reducing Toxin Load
Minimizing exposure to toxins in your environment can be crucial. Avoid secondhand smoke, polluted areas, and make your home toxin-free by addressing issues like mold, conventional cleaning products…Invest in water purification systems, opt for organic foods, and reduce plastic usage.
Detoxification
Toxins can accumulate in the body over time. Support your body’s natural detoxification processes by staying hydrated, considering infrared sauna sessions, ensuring proper dental care, and incorporating detoxifying foods and supplements like activated coconut charcoal.
Gut Health Support
Given the strong connection between gut health and colon cancer, it’s vital to assess your gut’s status. Tailoring your diet to support gut health and addressing gut infections under professional guidance is crucial.
Probiotics
Probiotics* play a pivotal role in maintaining gut health. Include probiotic-rich foods like sauerkraut and fermented vegetables in your diet, complemented by a high-quality probiotic supplement.
Vitamin D Optimization
Adequate vitamin D* levels are essential. Aim for regular sun exposure, incorporate vitamin D-rich foods, and consider supplementation to ensure optimal levels.
Comments
* Always consult a qualified naturopath for assessment of need and prescription of quality supplements.
There are additional options for addressing cancer naturally – one is called “Salvestrols” which are plant-derived substances that target only cancer cells by inducing apoptosis (cell death). These substances are found in organically grown fruit and vegetables but can be taken in a supplemental form. To learn more watch the videos: https://www.youtube.com/watch?v=B_5F9ampVjU and https://youtu.be/qDxROOUKrSc. For product information visit www.salvacare.co.nz
The other highly effective treatment involves frequency therapy. As there are many devices on the market, many of which are inferior, I only recommend one: the Ryfemax.
